Key Takeaways
- Menopause affects blood sugar regulation, not just sleep, mood, or temperature control.
- Glucose changes begin years before menopause is complete and are commonly mistaken for aging or lifestyle failure.
- Declining and fluctuating estrogen levels alter insulin sensitivity, liver glucose input, stress responses, and fat storage.
- Understanding glucose patterns, not chasing perfect numbers, helps support sustainable metabolic health through menopause.
that {{mid-cta}}
Menopause is very often associated with symptoms such as hot flashes, sleep disruption, and mood changes, but its effects on blood sugar are just as important while being less visible. Many women notice that foods they used to tolerate now cause spikes, and their energy feels less stable throughout the day.
All these changes can happen gradually, oftentimes years before a woman reaches post-menopause, and are frequently mistaken for simple aging or a lifestyle failure. In reality, menopausal changes in blood sugar are driven by physiological mechanisms. Declining and fluctuating estrogen alters the production, transport, and storage of glucose throughout the body.
Insulin sensitivity shifts, stress hormones exert a strong influence, and body composition changes can directly affect metabolic health as a whole.
Below, we will explain how menopause alters blood sugar regulation from the inside out. Every single section will introduce a glucose-related problem generally seen during perimenopause or menopause, explain why it happens, and then provide you with practical monitoring and management strategies.1
The goal isn’t to achieve perfect control over it, but to stay informed and develop ways to adapt your glucose management so that it remains sustainable for you in the long term.
The Hormonal Shift Behind Menopause Blood Sugar Changes
Estrogen is a core participant in metabolic regulation. It supports insulin sensitivity in muscle and liver tissue, helps suppress excessive glucose release from the liver, and influences how fat is stored and mobilized.
During perimenopause, estrogen does not decline smoothly; instead, levels fluctuate from cycle to cycle. Progesterone tends to decline earlier and more consistently, which creates a hormonal imbalance. By postmenopause, estrogen stabilizes at a much lower baseline.
These hormonal shifts will dictate how your body handles glucose at rest, after meals, and during stress. Understanding this will help explain why blood sugar patterns change even when diets and daily activities remain the same. The result is not a single change, but a chain of shifts that affect blood sugar throughout the day and night.
Rising Fasting Glucose During Menopause
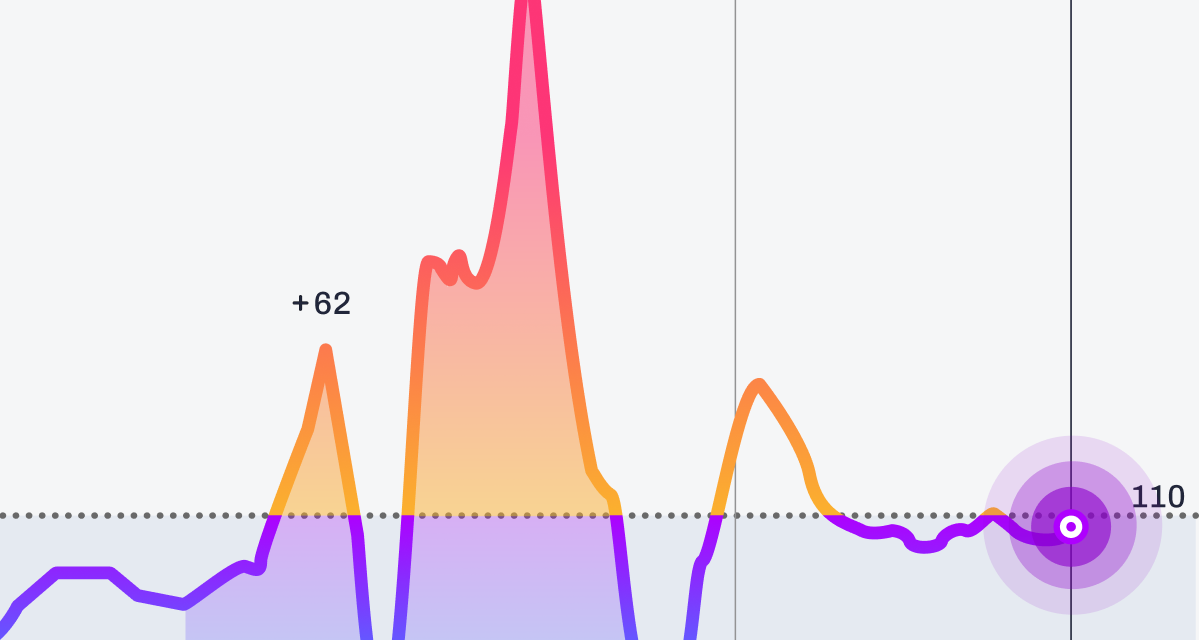
One of the earliest menopausal blood sugar changes many women notice is higher fasting glucose. Morning readings may go up despite unchanged eating habits or physical activity. This can often feel confusing because there might not be anything obvious that explains why the shift is happening in the first place.
Fasting glucose reflects overnight glucose production by the liver. Estrogen typically helps insulin reduce glucose release. However, when estrogen decreases, the liver becomes less sensitive to insulin's signals.2
A consistently elevated fasting glucose can, over time, increase strain on insulin-producing cells and contribute to cardiometabolic risk. Even small increases can signal early insulin resistance, especially with other menopausal changes. Elevated fasting glucose is also associated with increased inflammation and vascular stress, even before diabetes develops.
How to Recognize and Respond to Higher Morning Glucose
Managing rising fasting glucose begins with recognizing it as a hormonal and metabolic signal rather than a dietary failure. Tracking morning glucose over weeks will provide more insight than isolated readings.
Some good strategies to support overnight glucose regulation include consistent sleep timing, eliminating late-night heavy meals, and incorporating regular resistance training, which improves insulin sensitivity independent of estrogen.
Larger Post-Meal Blood Sugar Spikes
.png)
During perimenopause and menopause, meals that once elicited a consistent glucose response may now cause higher, longer-lasting spikes. This is especially noticeable after meals that include carbs.
Skeletal muscle is the main site for post-meal glucose uptake. Estrogen enhances insulin signaling in muscle tissue. This means that when estrogen declines, glucose uptake becomes less efficient, leading to more glucose circulating after each meal.
Repeated post-meal spikes also increase oxidative stress, inflammation, and accelerate your progression toward insulin resistance. They can also be heavily associated with energy crashes and increased hunger later in the day.
How to Structure Meals to Reduce Post-Meal Glucose Rises
Reducing post-meal spikes does not mean you have to eliminate carbs from your meals. Instead, focus on meal composition. Pairing carbs with protein, fiber, and fat will slow down absorption and lower peak glucose levels.
Light physical activity after meals can help muscles take up glucose through insulin-independent pathways. Tracking your blood sugar after meals helps you find the best foods for your body. This way, you can focus on what works for you instead of following general guidelines.
Increased Blood Sugar Variability
.png)
Many women experience unpredictable glucose responses during perimenopause. They can have the same meal multiple times, and it can produce different results on different days, not to mention that energy levels may feel unstable without any clear cause.
Hormonal fluctuations affect cortisol regulation.3 Cortisol directly raises blood sugar by stimulating glucose release from the liver. Generally, estrogen buffers cortisol’s effects, but this buffering weakens during perimenopause.
The result is increased glucose variability. Frequent ups and downs rather than a steady and easy-to-read pattern. High variability stresses metabolic systems. It raises cardiovascular risk, even with average glucose levels.
How to Stabilize Unpredictable Glucose Patterns
Stabilizing glucose variability requires you to look beyond the food you are consuming. Sleep quality, stress levels, and recovery all influence cortisol and glucose dynamics.
Tracking glucose alongside sleep and stress patterns helps identify triggers. Strategies that reduce physiological stress, such as adequate protein intake, consistent routines, and restorative movement, often improve variability more effectively than following a strict diet.
Declining Insulin Sensitivity
.jpeg)
As menopause progresses, many women develop reduced insulin sensitivity that does not respond quickly and effectively to calorie reduction or increased cardio exercise.
Estrogen supports insulin receptors efficiently. This means that when estrogen declines, cells require more insulin to move the same amount of glucose. The pancreas compensates for this by producing more insulin, which in turn promotes fat storage and worsens insulin resistance over time.
This drastic shift increases the risk of metabolic syndrome, type 2 diabetes, and cardiovascular disease while also making weight management a lot more difficult.
How to Support Insulin Effectiveness The Right Way
Improving insulin sensitivity during menopause requires focusing on muscle and metabolic health rather than weight alone. Resistance training increases muscle mass and glucose disposal capacity. A good protein intake promotes maintenance and growth while keeping you satiated.
Remember, monitoring insulin-related markers, not just glucose, can provide you with early insight into metabolic changes.
Central Fat Gain and Its Effect on Blood Sugar
Menopause is often accompanied by an increase in abdominal fat, even without overall weight gain. This change often coincides with worsening glucose control.
Visceral fat is metabolically active and releases inflammatory compounds that impair insulin signaling. As insulin declines, fat distribution shifts toward the abdomen, increasing insulin resistance and worsening blood sugar control.
This creates a reinforcing cycle where insulin resistance promotes fat storage, and visceral fat further impairs insulin sensitivity. Over time, this cycle increases cardiometabolic risk and contributes to persistent glucose elevation.
How Improving Body Composition Supports Glucose Control
Addressing body composition rather than weight alone is vital. Strength training, sufficient protein intake, and consistent glucose-friendly habits help reduce visceral fat over time.
Glucose monitoring can reveal whether fat gain is driven by insulin dynamics, which allows for better adjustments rather than generalized decisions that further hinder you.
Sleep Disruption and Overnight Glucose Changes
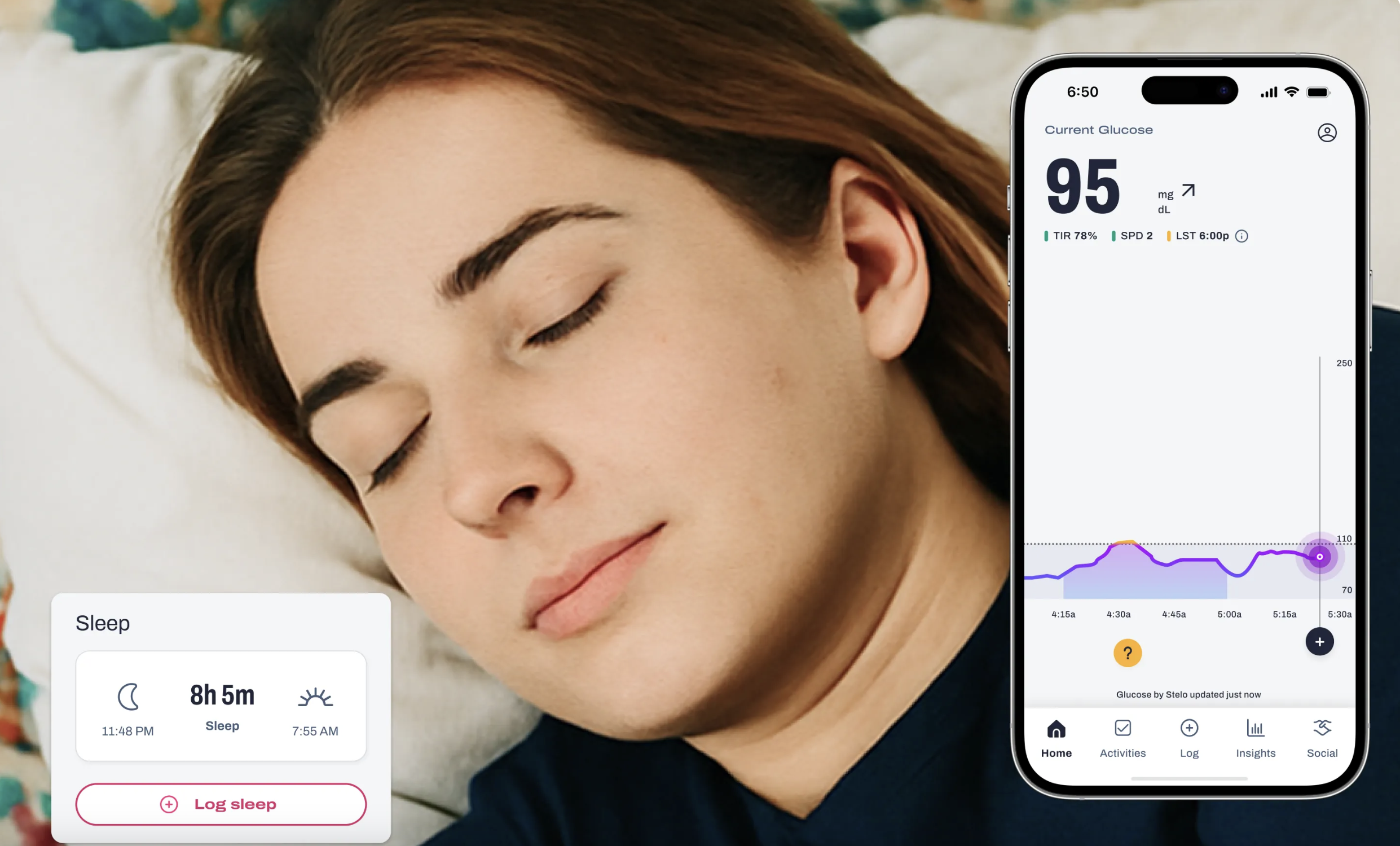
Sleep problems are common during menopause. They often happen with nighttime glucose issues. Some women experience elevated overnight glucose levels, while others may have nocturnal drops that severely disrupt sleep.
Poor sleep increases cortisol and reduces insulin sensitivity the following day. At the same time, circadian regulation of glucose becomes less stable as estrogen declines. Blood sugar swings can also disrupt sleep, which creates an unhealthy loop.
Chronic sleep-related glucose dysregulation contributes to higher long-term glucose markers and metabolic risks.
How Better Sleep Supports Overnight Glucose Regulation
By improving sleep quality, you support glucose regulation. Following consistent sleep schedules, balanced meals, and stress-reducing pre-bed routines helps stabilize overnight glucose.
When sleep issues persist, checking and reviewing nighttime glucose patterns can reveal whether blood sugar swings are contributing to your waking up, which helps guide you toward better strategies.
Long-Term Cardiometabolic Risk After Menopause
.jpeg)
Even subtle glucose changes during menopause can increase long-term cardiovascular and metabolic risks.
Postmenopausal glucose dysregulation directly contributes to vascular inflammation, arterial stiffness, and insulin resistance.4 Cardiovascular disease risk rises significantly after menopause, and glucose regulation plays a major role in this.
Since these changes develop over time, they are often overlooked until a disease is fully established.
How Early Glucose Awareness Helps Reduce Long-Term Risk
Early awareness and monitoring allow for prevention rather than reaction. By tracking glucose trends, insulin markers, and lipid profiles, you’re able to see a better picture of your metabolic health.
Lifestyle strategies that support glucose stability, muscle mass, and stress regulation form the foundation of long-term protection. All with clinical support when needed.
Appetite Dysregulation and Blood Sugar Signaling Changes
During menopause, many women notice stronger hunger signals, increased cravings, or difficulty feeling fully satisfied after meals. These changes often accompany blood sugar instability but are often attributed to poor willpower or habit changes.
Estrogen interacts with appetite-regulating hormones such as leptin5 and ghrelin6, as well as glucose-sensing neurons in the brain. As estrogen declines, satiety signals become less efficient, and blood sugar fluctuations provide a stronger influence on hunger perception.
When your glucose rises quickly and falls sharply, your brain interprets this as an energy shortage, which triggers cravings, particularly for fast-digesting carbs. Over time, this pattern will increase caloric intake, worsen glucose variability, and contribute to insulin resistance.
How Stabilizing Glucose Helps Regulate Hunger and Cravings
Stabilizing your appetite starts with stabilizing your glucose. Meals that emphasize protein, fiber, and slower-digesting carbs can reduce rapid glucose swings while supporting strong satiety signals.
Tracking glucose alongside hunger patterns can help distinguish physiological hunger from glucose-driven cravings. This sort of awareness lets you adjust your meal timing and composition proactively rather than reacting to cravings after they have escalated.
Stress Reactivity and Glucose Sensitivity
.png)
During menopause, blood sugar becomes a lot more sensitive to stress. Emotional stress, time pressure, and cognitive overload can all cause noticeable glucose elevations even without eating.
Cortisol increases glucose availability by stimulating hepatic glucose release. Estrogen normally moderates this whole interaction. But when estrogen declines, cortisol’s effects are amplified, leading to stress-induced hyperglycemia.
Frequent stress-driven glucose elevations contribute to different problems, such as fatigue, variability, and insulin resistance, while also masking the effectiveness of dietary changes.
How Managing Stress Improves Blood Sugar Responses
Managing stress is not optional for glucose stability during menopause; it is a metabolic intervention. Practices that reduce nervous system activation, such as controlled breathing, restorative movement, and predictable routines, all positively influence glucose patterns.
Using past and present glucose data to observe stress responses helps validate the role of stress and reinforces the importance of recovery strategies paired with nutrition and exercise.
Turning Menopause Blood Sugar Awareness into Action
Menopause blood sugar changes are not random, and they are definitely not a personal failure. They reflect a shift in hormonal signaling that alters glucose production, insulin sensitivity, and energy regulation.
By focusing on your specific patterns rather than perfection, and by using monitoring tools as feedback rather than judgment, you can adapt your habits to match your changing physiology.
Menopause represents a metabolic transition, not a loss of control. With informed strategies, glucose regulation can remain stable, supportive, and sustainable well after your menopausal years.
Menopause also requires recalibrating expectations. Strategies that worked before may become less effective or even counterproductive. Sustainable action means adapting your habits to hormonal reality rather than intensifying your efforts in the same direction.
Learn More With Signos’ Expert Advice
If you want to understand better how your daily habits influence your metabolic health, Signos offers expert-backed education and tools to help you build healthier routines. You can explore how glucose patterns connect to energy, hunger, and your overall well-being, and learn more about glucose levels through Signos’ blog.
Topics discussed in this article:
References
- Cleveland Clinic. (n.d.). Perimenopause. https://my.clevelandclinic.org/health/diseases/21608-perimenopause
- Mauvais-Jarvis, F. (2015). Estrogen and insulin resistance: Clinical implications. Journal of Endocrinology, 223(2), R49–R60. https://pmc.ncbi.nlm.nih.gov/articles/PMC4116406/
- Reaven, G. M. (2010). Insulin resistance and cardiovascular disease. Endocrine Reviews, 31(4), 364–395. https://pmc.ncbi.nlm.nih.gov/articles/PMC3079864/
- Santoro, N., Epperson, C. N., & Mathews, S. B. (2023). Hormonal changes and glucose metabolism during menopause. Frontiers in Endocrinology, 14, Article 12534243. https://pmc.ncbi.nlm.nih.gov/articles/PMC12534243/
- Hinkle, J. L., & Cheever, K. H. (Eds.). (2023). Physiology, estrogen. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK537038/
- Society for Endocrinology. (n.d.). Ghrelin. https://www.yourhormones.info/hormones/ghrelin/


.jpg)
.jpg)
.svg)


%20(1).jpg)

.jpg)


.webp)
.jpg)

















